Кроксы В последние годы кроксы заметно вернулись в массовую культуру, превзойдя свое скромное происхождение как функциональную обувь и став модным трендом. Эти необычные сабо, любимые одними и ненавидимые другими, вызвали

Кроксы В последние годы кроксы заметно вернулись в массовую культуру, превзойдя свое скромное происхождение как функциональную обувь и став модным трендом. Эти необычные сабо, любимые одними и ненавидимые другими, вызвали
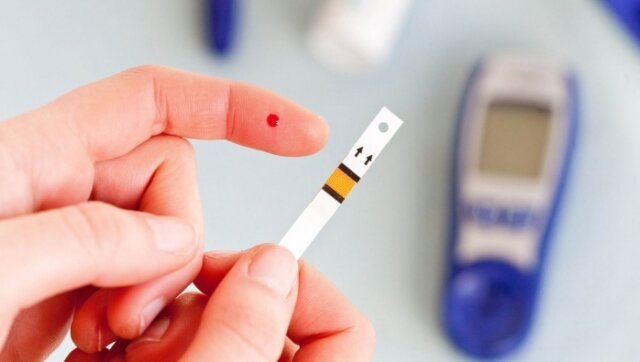
Диабет — одно из самых коварных заболеваний. Он может не только испортить качество жизни, но и сделать человека инвалидом. Диабет деструктивно воздействует на ткани и все сосуды. Тяжелые формы этого

После долгих лет заблуждений вам пора узнать, что стакан молока — не единственный способ получить здоровую дозу кальция. При этом кальций — чрезвычайно необходимый нашему организму минерал. «Кальций важен для

Интервальное голодание (IF) набирает популярность как метод снижения веса и улучшения здоровья. Эта модель питания включает в себя чередование периодов приема пищи и голодания либо путем ограничения приема пищи, либо

Благодаря выгодам, которые можно получить от использования оливкового масла для приготовления здоровой пищи и красоты, мы привыкли воспринимать этот продукт исключительно со знаком «плюс». Но, как бы там ни было,

Прийти в хорошую физическую форму важно не только для морального удовлетворения, но и для здоровья. Отложение жира в области живота и талии ведет к нарушению гормонального обмена, сдавливает внутренние органы

Возможно, вы заметили, что бокал вина по пятницам постепенно превратился в два или три в течение недели. Или вы просто хотите отказаться от алкоголя в рамках детокса и здорового образа

Очень многие, начиная правильно питаться, вскоре понимают, что их расходы на продукты значительно возросли. И, как результат, спешат с выводами, что здоровый образ жизни им не по карману. Полезные продукты

Септопластика – операция по исправлению носовой перегородки. Необходимость выпрямить перегородку обусловлена не только внешними дефектами, но и возможными последствиями для здоровья Cептопластика относится к хирургическому вмешательству, но при этом является

Чрезмерное количество сладкого в нашем рационе не только приводит к набору лишнего веса, но и нарушает нормальную работу обмена веществ, повышает риск развития сахарного диабета и других серьезных заболеваний. Отказ